
Have you ever heard of NOTES or TAMIS?
NOTES stands for natural orifice tansluminal endoscopic surgery and TAMIS stands for transanal minimally invasive surgery. Surgeon’s used to use flexible scopes to diagnose conditions and perform simple procedures like removing a foreign object, (a fish bone for example). Advances in technology and design of scopes have created a whole new approach to MIS (minimally invasive surgery).
We in CSSD need to be able to clean and sterilize the medical devices used to perform these types of surgery.
Advances in surgical techniques
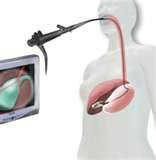 NOTES; is an alternative approach to conventional surgery. It is a combination of laparoscopic and endoscopic approaches to access the sterile peritoneal cavity via the mouth, anus or possibly the vagina. We have come to the point where high level disinfection of flexible scopes is simply not good enough. Spaulding taught us many years ago that an instrument that enters a sterile cavity must be sterile. Many of the new technologically advanced medical devices have complex designs and are heat and moisture sensitive, yet they need still need to be sterilized. The only way to sterilize these types of devices is to use a low temperature sterilization processes.
NOTES; is an alternative approach to conventional surgery. It is a combination of laparoscopic and endoscopic approaches to access the sterile peritoneal cavity via the mouth, anus or possibly the vagina. We have come to the point where high level disinfection of flexible scopes is simply not good enough. Spaulding taught us many years ago that an instrument that enters a sterile cavity must be sterile. Many of the new technologically advanced medical devices have complex designs and are heat and moisture sensitive, yet they need still need to be sterilized. The only way to sterilize these types of devices is to use a low temperature sterilization processes.
In SA we commonly use low temperature sterilizers to process or ‘reprocess’ heat sensitive ‘plastic’ type items. We reprocess single use devices opened in error and occasionally we reprocess ‘used’ single use devices.
Low temperature sterilizer’s can be used for so much more than just processing single use heat sensitive devices.
What can low temperature sterilizers do for you?
Reduce repair costs
In 2007 a hospital in Germany began sterilizing their rigid orthopaedic and urology scopes in a low temperature sterilizer. In 2009 they studied the frequency of repairs to those instruments processed in the low temperature sterilizer from 2007-2009. They compared it with frequency of repairs from 2005-2007. The results of the study were published in Central Sterilization, a CSSD orientated journal. They were able to reduce the number of monthly scope repairs of the orthopaedic instruments by 26% and urology instruments by 50%.
In SA we generally have a limited number of instrument sets and medical devices such as expensive orthopaedic drill sets. As a result staff ‘snatch’ drills as soon as the autoclave door opens, and take them to theatre (not allowing them to cool first). Once the set is opened in theatre staff wrap a wet swab around the hand piece to make it cool enough to handle. Handling hot medical devices straight from the autoclave is not best practice as it compromises sterility and may damage the drill.
Ensure Best Practice
Dancer (Dancer et al., 2012) recently published a study in the Journal of Hospital Infection called surgical site infections linked to contaminated surgical instruments. Instrument sets (orthopaedic) had been contaminated by micro-organisms found on the hands of staff. The staff handled the sets whilst they were still wet which created a portal for entry for the micro-organisms. Surely it would be much safer to process drills in a low temperature sterilizer at 50°C which are then available for immediate use.


